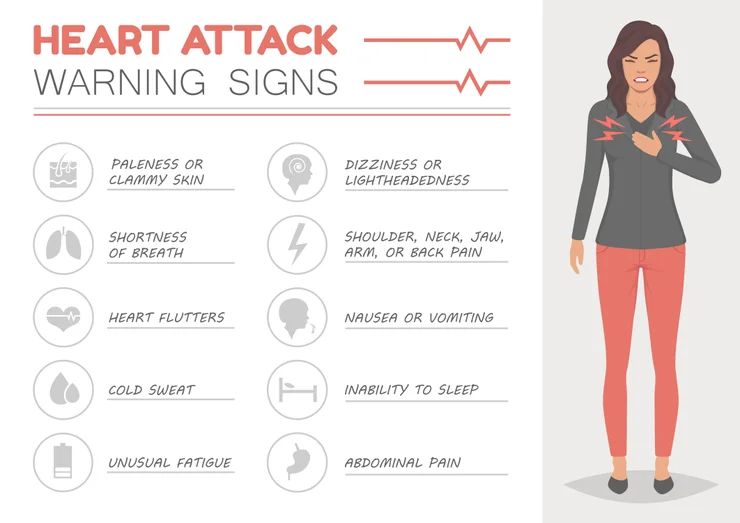
When Sarah felt an unusual wave of fatigue and nausea during her morning jog, she brushed it off as a stomach bug. Three hours later, she was in the emergency room having suffered a heart attack. At 52, she never imagined her heart was at risk. Like many women, Sarah didn't recognize the warning signs because they didn't match the chest-clutching symptoms she'd seen in movies.
Over 60 million women (44%) in the United States are living with some form of heart disease and it is the leading cause of death for women in the United States (1).
In 2023, it was responsible for the deaths of 304,970 women—or about 1 in every 5 female deaths (2). Yet despite these startling statistics, only about half (56%) of US women recognize that heart disease is their number 1 killer (3). Heart disease in women continues to be under-diagnosed, under-treated, and misunderstood. The reality is that women face unique cardiovascular challenges that are frequently overlooked by both patients and healthcare providers alike.